Dr. Graper and Dr. Harper – Breast Reconstruction Experts
Newer techniques, modifications in older techniques, and improvements in devices commonly used for reconstruction have led to more satisfied patients and surgeons. Women who seek breast reconstruction have more options now and should be educated on the risks and benefits of each possible reconstruction method when determining what’s best for them.
Women’s Health and Cancer Rights Act of 1998
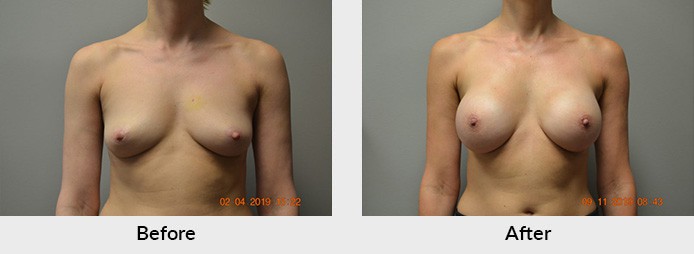
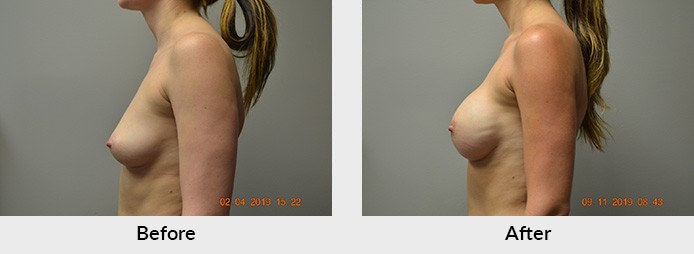
Outcomes-based research on the quality of life improvements and the psychological benefits associated with women who underwent breast reconstruction served as a stimulus for the Women’s Health and Cancer Rights Act that was signed into legislation in 1998. This act mandates that insurance companies cover not only breast and nipple reconstruction, but also procedures on the other breast like breast augmentation, breast lift, breast reduction, breast revision surgery, etc. in order to achieve symmetry. Additional legislation passed in 2001 actually imposes penalties on noncompliant insurers. All of this means that women that undergo breast surgery for cancer are guaranteed the option for breast reconstruction and surgery on the other breast to make them symmetrical. There is no timeframe set for this act. If you had surgery for breast cancer in the past and you either were not offered or chose to not undergo reconstruction, or perhaps you did and think you may need revisionary work, your surgery must be covered by your insurance company. It’s never too late to start your reconstruction process or revise previous work.
Breast Reconstruction
Breast reconstruction is broadly divided into two main categories. The first category involves reconstruction using only the patient’s natural tissues. This is referred to as “autologous reconstruction” and involves the transfer of tissue from one part of the body to the breast area to sculpt a new breast. Common areas used to transfer include the lower abdomen (known as the TRAM flap) and the back (known as the latissimus dorsi flap). There are a whole host of other areas that have been used for reconstruction including the buttocks and the upper medial thigh, but the TRAM and the latissimus dorsi are the two most common methods.
The second category of breast reconstruction is termed “device-based reconstruction” and involves the use of breast implants as the principal means of creating the new breast. This method of breast reconstruction is the most common statistically and the use of adjunctive techniques (such as autologous fat grafting and use of acellular dermal matrices) and newer, better devices have improved cosmetic outcomes. In most instances, a temporary device called a tissue expander is placed first. This allows the breast tissues to heal with less stress while maintaining a breast pocket that can be stretched over time and ultimately accommodate an implant. We then add fluid to the expander at your clinic appointments until we reach your goal size for your breasts. At a second operation, we will exchange the expander for a softer, more natural-appearing, and feeling implant. We can also do any adjunctive procedures or minor revisions at the time of that surgery, as well. For some women, the use of an expander is unnecessary and we are able to do a single-stage, “direct-to-implant” reconstruction. In this scenario, the new breast is immediately reconstructed with the more natural implant, often aided by the use of the acellular dermal matrices. Often, however, as your tissues heal and adapt to the new implant, revisions are necessary to achieve the optimal cosmetic result.
With either autologous or device-based breast reconstruction, it may take more than one surgery to achieve your and your plastic surgeon’s goals. Revisionary surgery is common and in some instances, should be the expectation.
Mastectomy and Partial Mastectomy (Lumpectomy) Options
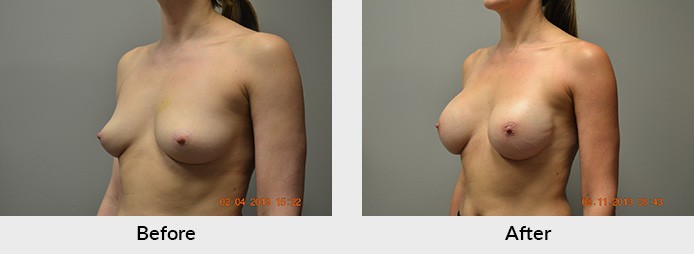
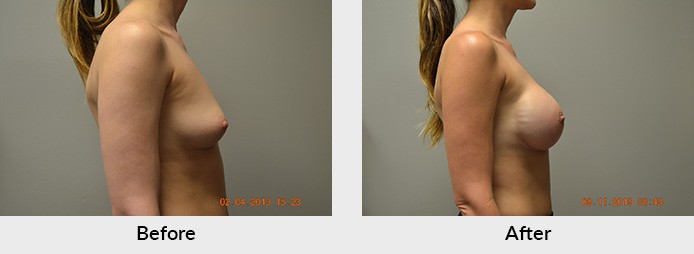
There has also been a continued evolution in breast cancer surgery. The advent of skin-sparing and now nipple-sparing mastectomies has improved cosmetic outcomes in patients who are candidates for those surgeries. Patients that decide to have breast conservation therapy (a combination of partial breast mastectomy or “lumpectomy” along with radiation therapy) also have more options. Oncoplastic breast surgery involves removing the cancerous tissue in a standard breast reduction technique. In women with larger breasts that would accommodate a reduction, symmetrical surgeries to both breasts can be performed at the same time. It may also make your subsequent radiation treatments easier, safer, and more efficacious. These options should be addressed with both your cancer surgeon and your plastic surgeon who should then communicate with each other in order to decide what’s best for you.
Timing of Your Reconstruction
The timing of your reconstruction depends on many factors. Most importantly, your preference should be considered. There are advantages and disadvantages to both an “immediate or delayed reconstruction” and those should be discussed at your initial consultation. The need for chemotherapy and especially radiation therapy may also play a big role in determining when it’s best to start your reconstruction. An open discussion with and between all of your cancer doctors (plastic surgeon, cancer surgeon, radiation oncologists, and medical oncologists) should be done to help make this decision. Timing of reconstruction will not affect your insurance covering these procedures but may affect the quality of your outcome.
Which Options Are Right For You?
The important thing to remember is that your breast reconstruction is exactly that — yours. As each woman is different, so is her body, her desired outcome, her idea of beauty, her concerns, and her goals. Your plastic surgeon should help guide you through the decision process, but ultimately, the decision is yours. That being said, not every woman is a good candidate for every type of breast reconstruction. Likewise, not every plastic and reconstructive surgeon is great at every technique. You and your plastic surgeon should discuss every option, weigh the risks and benefits, and decide on the best option for you.




